
Understanding Prostatitis: A Comprehensive Guide for Patients by Mr. Angus Campbell
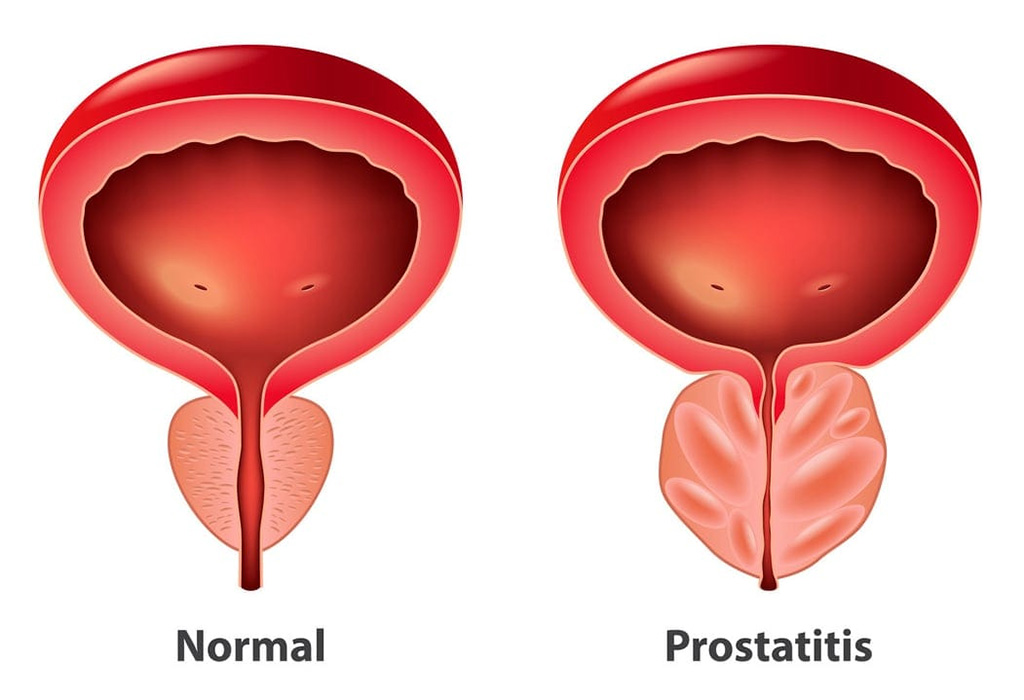
Prostatitis, an inflammation of the prostate gland, is a common condition affecting men across various age groups. It can be caused by infections, structural abnormalities, or even stress, and it significantly impacts a man’s quality of life. This guide will help you understand the types, causes, symptoms, and treatment options for prostatitis, presented in a patient-centered, easy-to-digest format.
What is Prostatitis?
The term "prostatitis" combines "prostate" (referring to the prostate gland) and "-itis" (indicating inflammation). This condition involves inflammation of the prostate gland, which is located just below the bladder and surrounds the urethra. Prostatitis can have infectious or non-infectious origins, making its diagnosis and treatment a multifaceted process.
Epidemiology
Prostatitis affects about 10-12% of the male population.
It is most common in younger and older men, with middle-aged men being less frequently affected.
Causes and Risk Factors
1. Structural Abnormalities
Bladder Outlet Obstruction: Often due to an enlarged prostate (Benign Prostatic Hyperplasia or prostate cancer).
Kidney Stones: Stones lodged in the urinary tract can increase the risk of infection and inflammation.
2. Infections
Urinary Tract Infections (UTIs): Bacteria ascending from the urethra can infect the prostate.
Sexually Transmitted Infections (STIs): Unprotected sexual intercourse increases the risk of infections like gonorrhea or chlamydia.
3. Medical Interventions
Catheters: Bacteria can travel along a catheter to infect the prostate.
4. Immune and Lifestyle Factors
Immunosuppression: Conditions like diabetes, AIDS, or advanced age can weaken the immune system.
Stress: Prolonged stress can reduce immunity and contribute to prostatitis.
Types of Prostatitis
Prostatitis is categorized into four main types based on its cause and presentation.
Type 1: Acute Bacterial Prostatitis (ABP)
Cause: A sudden bacterial infection, often stemming from an ascending UTI.
Common Bacteria: E. coli, Klebsiella, Proteus, Pseudomonas, Serratia, and STIs like gonorrhea and chlamydia.
Symptoms: Fever, chills, body aches, malaise, urinary urgency, frequency, burning during urination (dysuria), and pelvic pain.
Type 2: Chronic Bacterial Prostatitis (CBP)
Cause: Persistent bacterial infection, often following an acute episode.
Mechanism: Bacteria form biofilms in the prostate, protecting them from antibiotics and immune responses.
Symptoms: Long-lasting or recurring pelvic pain, urinary discomfort, pain during or after ejaculation, sexual dysfunction, and potential infertility.
Type 3: Chronic Pelvic Pain Syndrome (CPPS)
Cause: Non-infectious inflammation, often due to urine reflux into the prostate.
Symptoms: Chronic pelvic pain, discomfort in the penis, scrotum, or perineal area, and urinary retention.
Type 4: Asymptomatic Inflammatory Prostatitis
Characteristics: No symptoms despite prostate inflammation, often detected during examinations for other conditions.
Diagnosis
Diagnosing prostatitis involves a combination of medical history, physical examination, and laboratory tests.
1. Medical History
Your doctor will ask about symptoms, sexual activity, past infections, and urinary habits.
2. Physical Examination
Digital Rectal Exam (DRE): To assess the prostate for tenderness or swelling.
3. Laboratory Tests
Urinalysis and Urine Culture: To identify bacteria or signs of infection.
STI Testing: To rule out sexually transmitted infections.
Complete Blood Count (CBC): To detect signs of systemic infection.
4. Imaging
Trans-Rectal Ultrasound (TRUS): Helps visualize an inflamed prostate.
CT Scan: Used to identify complications like abscesses, especially in immunocompromised patients.
Treatment Options
For Bacterial Prostatitis (Type 1 and 2)
Antibiotics:
Fluoroquinolones, macrolides, or tetracyclines are commonly used due to their ability to penetrate prostate tissue.
Treatment duration is typically longer (4–6 weeks) than for other infections to ensure complete eradication.
Surgical Drainage: Required for abscesses detected on imaging.
For CPPS (Type 3)
Treatment follows the UPOINT system, addressing various aspects of the condition:
U (Urinary): Alpha-blockers like tamsulosin improve urinary flow and reduce reflux.
P (Psychosocial): Stress and anxiety management.
O (Organ-Specific): Anti-inflammatory supplements like quercetin to reduce prostate inflammation.
I (Infection-Related): Antibiotics may be considered if a bacterial component is suspected.
N (Neurologic): Medications like pregabalin can help manage nerve-related symptoms.
T (Tenderness): Pelvic floor physical therapy alleviates muscle tension and associated pain.
Managing Prostatitis: Practical Tips
Hydration: Drink plenty of water to flush the urinary tract.
Hygiene: Maintain cleanliness to prevent infections.
Stress Management: Incorporate relaxation techniques like mindfulness or yoga.
Follow Treatment Plans: Complete prescribed medications and attend follow-up appointments.
Conclusion
Prostatitis is a multifaceted condition that can range from acute bacterial infections to chronic pelvic pain syndromes. While it can be challenging to manage, understanding its types, causes, and treatment options empowers patients to take control of their health.
If you experience symptoms or have concerns about prostatitis, consult a healthcare provider promptly for a thorough evaluation and personalized care.
FAQs About Prostatitis
Q1: What are the main symptoms of prostatitis?
A: Prostatitis symptoms vary depending on the type but commonly include pelvic pain, frequent or urgent urination, burning during urination, pain during ejaculation, and discomfort in the lower abdomen, penis, or perineum. Acute cases may also present with fever, chills, and body aches.
Q2: Is prostatitis a common condition?
A: Yes, prostatitis affects about 10–12% of the male population. It is particularly common in younger men under 50 and older men over 60, often due to different risk factors such as infections or an enlarged prostate.
Q3: How is prostatitis diagnosed?
A: Diagnosis involves:
A detailed medical history and physical exam, including a digital rectal exam (DRE).
Laboratory tests like urinalysis, urine cultures, and STI testing.
Imaging, such as a trans-rectal ultrasound or CT scan, to assess complications like abscesses.
Q4: Is prostatitis contagious?
A: Prostatitis itself is not contagious. However, if caused by a sexually transmitted infection (STI) like gonorrhea or chlamydia, the underlying infection can be transmitted through unprotected sexual contact.
Q5: Can prostatitis affect fertility?
A: Chronic bacterial prostatitis and chronic pelvic pain syndrome (CPPS) can impact fertility due to inflammation and potential damage to the prostate and surrounding tissues. Proper treatment can help mitigate these effects.
Q6: What are the long-term effects of untreated prostatitis?
A: If left untreated, prostatitis may lead to complications such as chronic pain, recurrent infections, urinary retention, or the development of abscesses. In rare cases, untreated acute bacterial prostatitis can lead to sepsis, a potentially life-threatening condition.
Q7: Can prostatitis be cured?
A: Many cases of bacterial prostatitis can be cured with appropriate antibiotic treatment. Chronic forms, particularly CPPS, may not have a definitive cure but can be effectively managed with a combination of medications, physical therapy, and lifestyle changes.
Q8: What lifestyle changes can help manage prostatitis?
A:
Stay hydrated and maintain a healthy diet.
Avoid triggers like alcohol, caffeine, and spicy foods.
Practice stress management techniques.
Perform pelvic floor relaxation exercises if advised by a physical therapist.
Q9: Should I avoid sexual activity if I have prostatitis?
A: It depends on the type and severity. Acute bacterial prostatitis may require abstinence until the infection is treated. Chronic forms, like CPPS, generally don’t require abstinence, but you should consult your healthcare provider for personalized advice.
Q10: When should I see a doctor?
A: See a doctor if you experience:
Persistent pelvic pain or urinary symptoms.
Fever and chills along with urinary discomfort.
Pain during ejaculation or significant sexual dysfunction.
Prompt evaluation and treatment can prevent complications and improve quality of life.
